|
|
| A message from Titanic |
|
|
SHELDON H. PRESKORN, MD
|
|
Journal of Practical Psychiatry and Behavioral Health, July 1998; 4:236-242
|
Thanks to James Cameron, the story of the Titanic has become a common cultural experience around the world. Most of us have vicariously experienced the horror of the crew in the crow's nest and on the bridge as they see the iceberg dead ahead in their path. Although the orders have been given to reverse the engines and turn hard to port, Titanic remains on her fatal collision course. Why didn't the ship turn in time? Inherent in the answer to this question and others about the Titanic is a message for every clinician who prescribes medications. In this column, I will use an actual case to illustrate the Titanic's message.
THE CASE
A 67-year-old female with Parkinson's disease had been successfully treated with selegiline (L-deprenyl), 10 mg/day, and trihexyphenidyl, 3 mg/day. Fluoxetine, 20 mg/day, was added to her regimen for the apparent development of a depressive episode. However, the patient became agitated. Hence, lorazepam, 2 mg/day, was added. Yet she became more combative, confused, and suspicious and began to complain that people were talking about her. For that reason, lorazepam was stopped and haloperidol, 4 mg/day, was started. Within a few days, the patient became rigid to the point of being virtually mute and catatonic. On 8/21/97, she was hospitalized.
The physical examination on admission was consistent with severe Parkinsonism but revealed no other abnormality. Mental status examination found auditory and visual hallucinations involving little children and significant deficits in recall and attention. She was not oriented to person or place and reported depressed mood, insomnia, poor appetite, and lack of energy.
Laboratory evaluation included a chemistry-25 profile, a urinalysis including a screen for drugs of abuse, a complete blood count, thyroid function tests, an electrocardiogram, and magnetic resonance imaging of the brain. The results were all within normal limits except a finding of leukocytes and bacteria in her urine. She was asymptomatic for a urinary tract infection (UTI).
Haloperidol was stopped at admission. The next day, fluoxetine was stopped due to a pharmacy alert and risperidone, 0.5 mg b.i.d., was started for her psychotic symptoms. On 8/23/97, a consultant started ciprofloxacin for her asymptomatic bacteriuria. On 8/26/97, risperidone was stopped due to excessive sedation. After completion of the ciprofloxacin, olanzapine, 2.5 mg b.i.d., was started. Over the next 2 weeks, the patient's psychosis slowly resolved. Her confusion also improved but did not fully resolve. Her Parkinsonian symptoms became much less pronounced. In fact, she improved to the point that plans for discharge to a nursing home were canceled and she was discharged back home to her family.
What happened?
For those readers who are in the mood for a clinical game of "what happened?", take a moment to list all the factors you would want to consider had you been consulted about this patient's management by her attending physician. To assist in this process, Figure 1 shows the time course for the various medications that this patient received.
| Figure 1. Time Course of Medications | 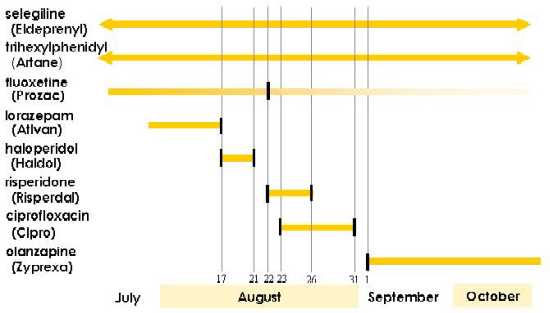 |
Regular readers know that we approach such questions from the perspective that drug response is a function of three variables as summarized by Equation 1 below:
| Response | = | pharmacodynamics | | | x pharmacokinetics | | | x biological variance (Equation 1a) | | or | | | | Response | = | affinity for site(s) of action | | | x drug concentration | | | x biological variance (Equation 1b) |
The biological variance term in equation 1 includes the diagnosis for which the medication is prescribed, other concomitant illnesses, genetics, gender, and the internal environment of the body. All these factors can shift the dose-response curve for the patient. Physicians need to keep all these factors in mind but particularly the internal environment, because they play a significant role in determining that internal environment via their medication recommendations.
Let us now examine this case from the perspective of Equation 1.
Dopamine Receptor Blockade
The proximal cause of this patient's hospitalization was a drug-disease interaction. The patient had Parkinson's disease, which fits under the biological variance term in the above equation. While Parkinson's disease was not the target illness for which fluoxetine, lorazepam, and haloperidol were added, it played an important role in the patient's course as explained below.
Parkinson's disease is characterized by a progressive loss of dopamine neurons in the substantial nigra and consequent dopamine denervation of the basal ganglia. In order to enhance the survival of our species, we are born with excessive capacity in many of our organs. This is true for our dopamine neurons just as it is for our kidneys and liver. Patients do not become clinically symptomatic from Parkinson's disease until they have lost approximately 70% of their original supply of dopamine neurons. Patients who have lost an appreciable number of dopamine neurons are biologically predisposed to extrapyramidal adverse effects when given dopamine receptor blockers, such as haloperidol, because they do not have the functional capacity to compensate for the blockade. That is true even if the patient has not yet lost enough dopamine neurons to have clinically symptomatic Parkinson's disease. Patients who are already symptomatic, like the one in this case, are generally exquisitely sensitive to dopamine antagonism.
While the haloperidol-Parkinson's disease interaction was the proximal cause of this patient's hospitalization, the question remains: What caused the deterioration that led the physician to prescribe first lorazepam and then haloperidol?
Why The Pharmacy Alert?
The hospital pharmacy's computer flagged the fact that the patient was on the serotonin reuptake inhibitor (SRI), fluoxetine, and the monoamine oxidase (MAO) inhibitor, selegiline. Such drugs used in combination can cause a serotonin syndrome (Table 1).1,2 The risk of this syndrome is probably less likely with the relatively selective MAO-B inhibitor, selegiline, than with nonselective MAO-A and B inhibitors such as phenelzine and tranylcypromine. Nevertheless, serotonin syndromes have been reported in patients taking selegiline and fluoxetine.1,2 In fact, the manufacturer has recently issued a warning against using selegiline and SRIs together to avoid such an interaction.2 Certainly, this patient's combativeness, confusion, and psychosis were consistent with a mild variant of the serotonin syndrome.3
| Table 1. Serotonin Syndrome: Signs and Symptoms | | | | Psychiatric | Cardiovascular | | Confusion | Tachycardia | | Disorientation | Hypotension | | Dysphoric mood | Cardiovascular collapse | | Hypomania | Death | | Racing thoughts | | | Pressured speech | Gastrointestinal | | Abdominal cramping | | Neurological | Bloating | | Tremulousness | Diarrhea | | Incoordination | | | Dysarthria | Other | | Myoclonus | Diaphoresis | | Hyperreflexia | Hyperthermia | | Headache | | Source: Sternbach H. The serotonin syndrome. Am J Psychiatry 1991;148:705-13. |
With such a trigger, a chain of events was set off that was reminiscent of the poem about the loss of the kingdom for want of a nail. In this case, the patient's worsening psychiatric status most likely resulted from a fluoxetine-selegiline interaction, which in turn led to the use of lorazepam. The failure of lorazepam in turn led to the use of haloperidol. Lorazepam may not only have been ineffective but may even have exacerbated the problem by causing behavioral disinhibition and increasing the patient's confusion. The abrupt discontinuation of lorazepam could have aggravated the situation by inducing a mild benzodiazepine withdrawal syndrome. The addition of haloperidol then severely worsened the patient's Parkinsonian symptoms-which led to her $20,000 hospitalization (i.e., from the nail to the kingdom).
As a result of the pharmacy alert, the physician immediately stopped the fluoxetine. But was the problem solved with that action? Before addressing this question, let's talk about the results of the laboratory tests and how they could affect the treatment of this patient.
The Laboratory Tests:
Which Ones, Why, and What Do They Add?
The physician ordered a chemistry-25 profile, a urinalysis including a urine screen for drugs of abuse, a complete blood count, and a complete thyroid panel. Would you have ordered any other laboratory tests, and why? What was learned from those that were ordered?
The initial lab results ruled out several potential confounding problems, such as an electrolyte imbalance. They also identified an asymptomatic bacteriuria, which might have contributed to the patient's declining cognitive status. However, that seems unlikely since her improvement did not follow a time course consistent with the sterilization of her urine and she has subsequently had recurrence of her asymptomatic bacteriuria without deterioration in her cognitive status.
Nevertheless, the finding of a bacteriuria on this hospitalization led to a consult and subsequently to treatment with ciprofloxacin. Beyond the sterilization of her urine, did the addition of that antibiotic have any other effects that the physician would want to keep in mind in treating the patient? Before we address that question, was there any other test you would have ordered if you had been the treating physician or consultant?
In this case, a fluoxetine level was ordered. Why? The consulting physician knew that fluoxetine was a Titanic-like drug in that, once started, it could not be quickly changed. Moreover, he knew that the effects of fluoxetine on the serotonin uptake pump and on several cytochrome P450 enzymes are concentration- dependent (i.e., the higher the concentration of fluoxetine/norfluoxetine, the greater its effect). The fact that these concentration-dependent effects would persist as long as fluoxetine and its active metabolite, norfluoxetine, persisted in the body needed to be taken into account in evaluating the treatment strategy for this patient. In other words, the serotonin syndrome resulting from the combined use of fluoxetine and selegiline would not resolve immediately after the discontinuation of fluoxetine.
Remember the Titanic hit the iceberg even though the ship had been turned hard to port over a mile away. Like the Titanic, a pivotal issue in this case was the lag between the time of the order to change course and the time that a meaningful change would actually have occurred. In other words, how long did it take to drop the patient's fluoxetine and norfluoxetine levels to a point where they were not pharmacologically relevant? What would you guess?
The answer turned out to be well over 1 month (Figure 2). In the case of the Titanic, part of the problem was the momentum of the ship (i.e., its mass x its velocity). Another factor was the Titanic's poor turning radius. The greater the turning radius, the more distance the ship would transverse before changing its course. The half-life of fluoxetine and norfluoxetine is like the turning radius of the Titanic: it determines how rapidly a midcourse correction can be made. The total level of fluoxetine plus norfluoxetine is like the momentum of the Titanic-the higher the level, the longer it will take to drop to a level that is pharmacologically inconsequential.
In this 67-year-old woman, the combined level of fluoxetine and norfluoxetine on 8/24/97 (i.e., 48 hours after the fluoxetine was stopped) was 390 ng/ml (Figure 2), twice the average level expected on a dose of 20 mg/day.4-6 In other words, this patient cleared fluoxetine twice as slowly as the usual patient on 20 mg/day.
As regular readers of this column know,
Concentration = dosing rate / clearance (Equation 2).
That means that the interval necessary to clear fluoxetine will be even longer in this patient than in the usual patient due to her slow clearance. In fact, 1 month after fluoxetine was discontinued she had the same total level we would expect in the average person currently taking 20 mg/day, and would consequently experience the same effects we would expect in the average person on 20 mg/day. Table 2 lists the major pharmacological effects that would have been expected in this patient as a result of the medications that were part of her internal environment while she was hospitalized.
Her total fluoxetine plus norfluoxetine level also meant that this patient had more serotonin uptake inhibition and more inhibition of CYP enzymes than occurs in the usual patient on 20 mg/day.5,6 In fact, the magnitude of these effects produced by fluoxetine in this patient would be virtually the same as would be expected in the average patient on 40 mg/day. On 20 mg/day, the average patient achieves approximately 80% serotonin uptake inhibition and substantial inhibition of two drug metabolizing cytochrome P450 (CYP) enzymes: CYP 2D6 and CYP 2C19.5-7
Some background is helpful to understand the magnitude of the inhibition of CYP 2D6 and CYP 2C19. These two CYP enzymes are genetically polymorphic.5 While the majority of people have normal copies of these enzymes and are called extensive metabolizers (EMs), a small percentage of the population has a defect in the genes for one or the other of these two CYP enzymes. These individuals are therefore deficient in either CYP 2D6 or CYP 2C19 and are termed poor metabolizers (PMs). Drugs normally dependent on these CYP enzymes for their clearance accumulate to an unusually high degree in PM individuals. These two independent gene defects are examples of genetically determined biological variance (i.e., the third variable in Equation 1). It turns out that a drug like fluoxetine can pharmacologically convert EMs to phenocopies of PM status by competitively inhibiting CYP 2D6 and CYP 2C19.5-8 In such a case, fluoxetine alters the internal environment of the patient so that other drugs dependent on these CYP enzymes for their clearance accumulate to an unusual extent relative to the dose given (i.e., Equation 2).
The typical total levels of fluoxetine plus norfluoxetine achieved on 20 mg/day will convert approximately 63% of CYP 2D6 EMs and 50% of CYP 2C19 EMs to phenocopies of PM status via these two respective enzymatic pathways.6,7 Since the extent of CYP enzyme inhibition is a function of the level of the inhibitor, the unusually high accumulation of fluoxetine and norfluoxetine in this patient increased the likelihood of such a conversion. Fluoxetine at the levels achieved in this patient will convert approximately 95% and 80% of CYP 2D6 and CYP 2C19 EMs to PM status, respectively.6,7 In addition, fluoxetine in the average individual on 20 mg/day will produce mild inhibition of CYP 3A3/4, as shown by an increase of approximately 30% in the levels of coprescribed alprazolam.5 Given the concentration-dependent nature of such inhibition, this patient would be expected to have had somewhat more than mild inhibition of CYP 3A3/4.
What Is the Significance of the Serotonin Uptake Inhibition and the CYP Enzyme Inhibition?
The greater degree of serotonin uptake inhibition that occurred in this patient as a result of the increased accumulation of fluoxetine increased the likelihood that she would experience at least a mild variant of the serotonin syndrome. For the same reason, she would have experienced more aggravation of her Parkinsonian symptoms since serotonin has an inhibitory effect on dopamine cell firing in the brainstem.9 Thus, fluoxetine, like any SRI, would have pharmacodynamically interacted with haloperidol to antagonize dopamine function in her basal ganglia. In addition, by inhibition of CYP 3A3/4, fluoxetine may have modestly increased the haloperidol accumulation, resulting in a greater degree of dopamine blockade in her basal ganglia. Thus, this patient likely had combined pharmacodynamic and pharmacokinetic interactions between fluoxetine and haloperidol which in turn aggravated the haloperidol-Parkinson's disease interaction we discussed initially.
The interaction between fluoxetine and selegiline may also have gone beyond a pure pharmacodynamic interaction. In 1992, the possibility was raised that fluoxetine might inhibit the demethylation of segeline based on a case report similar to the one presented here.1 In 1994, segeline was shown to be a substrate for CYP 2D6.10 Thus, fluoxetine, by its ability to substantially inhibit CYP 2D6, would be expected to have increased segeline accumulation, which in turn would have increased the segeline-induced inhibition of MAO-B. Moreover, segeline at higher levels loses its selectivity and inhibits MAO-A as well as MAO-B.4 Thus, it is likely that fluoxetine interacted both pharmacodynamically and pharmacokinetically with segeline. Of interest, the majority of the interactions that have been reported between SSRIs and segeline have involved fluoxetine, but that may be a function of its widespread use.
What about the Ciprofloxacin?
Ciprofloxacin is an antibiotic. However, it also inhibits the drug metabolizing enzyme, CYP 1A2.11,12 The addition of ciprofloxacin in a patient who had persistent, pharmacodynamically relevant levels of fluoxetine and norfluoxetine means that this patient would have had compromised ability to metabolize drugs via CYP 1A2, as well as CYP 2C19, CYP 2D6, and CYP 3A3/4 (Table 2). These effects on drug metabolizing CYP enzyme function were added to whatever other factors caused this patient to be a slow metabolizer of fluoxetine in the first place, probably some decreased hepatic arterial blood flow due to compromised left ventricular cardiac function plus mild age-related decline in hepatic and renal function. For all these reasons, the physician had to be cautious about which drugs were prescribed for this patient and at what doses since she would be likely to develop higher than usual levels (Equation 2), which would produce greater effects (Equation 1). Moreover, she was already fragile because of her age and medical illness and therefore would be more sensitive to any untoward consequence resulting from such increased drug accumulation.
| Table 2. Magnitude of Pharmacologic Effects in this Patient | | Effect | Magnitude | Drug Responsible | | Serotonin uptake inhibition | substantial | fluoxetine | | MAO inhibition | B >> A | selegiline | 5-hydroxytrytophamine-2A
(5-HT2A) and dopamine
(DA) receptor blockade | 5-HT2A > DA | risperidone | Muscarinic cholinergic
receptor blockade | unknown | trihexyphenidyl | | CYP 1A2 inhibition | moderate | ciprofloxacin | | CYP 2C19 inhibition | substantial | fluoxetine | | CYP 2D6 inhibition | substantial | fluoxetine | | CYP 3A3/4 inhibition | > mild | fluoxetine |
Ironically, the untoward consequences of drug-drug interactions can be misattributed to a worsening of the patient's underlying medical illness rather than being recognized as the result of a drug-drug interaction.9 That is precisely what happened in this case. The patient's deteriorating mental status was initially attributed to the development of a dementia-Parkinson's complex, Diffuse Lewy Body disease. As a result, plans were initially made to send her to a nursing home. Interestingly, 3 months after the discontinuation of fluoxetine, the patient's antipsychotic therapy was stopped without any return of psychotic symptoms and without any other deterioration in her mental status.
During her hospitalization, "atypical" antipsychotics were selected for this patient because they are less likely to aggravate Parkinsonian symptoms, presumably due to their blockade of the serotonin-2A receptor.4 However, there were problems with both olanzapine and risperidone. Olanzapine is dependent on CYP 1A2 for its clearance, and that CYP enzyme was likely partially inhibited by ciprofloxacin. Risperidone is converted to 9-hydroxyrisperidone by CYP 2D6, which would have been substantially inhibited by fluoxetine/norfluoxetine. On the other hand, 9-hydroxyrisperidone is dependent on CYP 3A3/4, which was likely only mildly inhibited by fluoxetine/norfluoxetine. Quetiapine is also metabolized by CYP 3A3/4 and was another option for this patient. In fact, it arguably could have had the least potential to aggravate her Parkinson's disease. However, quetiapine also blocks alpha-1 adrenergic receptors, which could lead to orthostatic hypotension-which would have been problematic in a patient already susceptible to falls as a result of her Parkinson's disease and osteoporosis (a gender-based biological variance factor in Equation 2). Also, quetiapine was new at the time and had not yet been used in such patients. We generally prefer to learn about the warts of new drugs by reading about them in the literature, unless we are doing a specific study designed with adequate safeguards to monitor the risks.
After all these considerations were weighed, the decision was made to go with risperidone but to keep the dose low and monitor for adverse effects, realizing they could present as a worsening of the patient's underlying neuropsychiatric illnesses. When the patient proved to be sensitive to even 1 mg/day of risperidone, she was switched to a low dose of olanzapine after the ciprofloxacin course was completed.
So How Long Did It Take to Change Course?
This case helps us empathize with the crew of the Titanic as they watched it sail into the iceberg despite their best efforts. As mentioned above, 1 month after stopping fluoxetine, the patient's norfluoxetine level was equal to the usual combined levels of fluoxetine and norfluoxetine in a patient taking 20 mg/day of fluoxetine (Figure 2). The norfluoxetine levels are important because norfluoxetine is equipotent or more potent than fluoxetine in terms of serotonin uptake inhibition and CYP enzyme inhibition.5,7 For this reason, 1 month after the discontinuation of fluoxetine, this patient would still have been expected to have approximately 80% inhibition of serotonin uptake and substantial inhibition of CYP 2D6 and CYP 2C19. Therefore, the prescribers still needed to be concerned about what other medications (and what doses) were selected for this patient.
THE ICEBERG
CYP enzyme mediated drug-drug interactions share some similarities with the Titanic's antagonist, the iceberg. First, 80% of the oxidative metabolism of commonly used prescription drugs is below the water line of our knowledge.13 Ironically, we know more about the oxidative metabolism of very recently released drugs than we do about older medications because CYP enzyme screening is now part of the drug development process.13,14 For that reason, it is wise to be cautious when selecting doses for a patient on a drug that is known to inhibit a CYP enzyme unless you know that drug is not metabolized by that CYP enzyme.
Trihexyphenidyl is an example of an older drug for which metabolic pathways have not been established. Thus, an unanswered question is: What role, if any, did trihexyphenidyl play in this patient's deterioration? Certainly, trihexyphenidyl can cause a central anticholinergic delirium via its receptor antagonism. However, the patient was on the same dose both before and after treatment with fluoxetine without experiencing a delirium. Since we do not know how trihexyphenidyl is metabolized, we do not know whether its clearance was altered by the co-administration of fluoxetine. Nevertheless, this explanation seems unlikely because the patient did not have an elevation of her pulse or the other stigmata of anticholinergic toxicity (e.g. "dry as a bone"). An additional unanswered question is whether there was any metabolic interaction between ciprofloxacin and fluoxetine or selegiline.
Another similarity between the iceberg and drug-drug interactions is the problem of distinguishing them from the background. In the case of the Titanic, the iceberg was both submerged and blue in hue. Those facts coupled with the calm sea made it difficult for the crew in the crow's nest to distinguish the iceberg from the blue backdrop of sea and sky. In the case presented here, the adverse consequences of drug-drug interactions were difficult to distinguish from the the patient's underlying health problems. In fact, the worsening of her mental status was initially interpreted as a worsening of her Parkinson's disease and treated as such.
THE CAPTAIN OF THE SHIP
The outcome of treatment, like the voyage of the Titanic, depends on the knowledge, awareness, and skill of the skipper. Captain Smith was an experienced seaman but had never commanded a ship as big as the Titanic. Apparently, he had not adequately field tested the ship and was therefore unaware of her poor maneuverability. Although he thought he would have plenty of time to avoid problems, he was fatally wrong. His confidence in his own and his ship's abilities contributed to his failure to take proper precautions.
Hopefully, case discussions such as this one can help physicians avoid untoward consequences as they navigate the sometimes treacherous waters of clinical care. In terms of field testing your knowledge of fluoxetine and norfluoxetine, how well did you do in terms of estimating the time needed for their washout and of knowing the pharmacological consequences of having a combined level of 390 ng/ml?
CONCLUSION
There are several take-home messages from this column. One is that the consequences of a drug-drug interaction can be seen but the cause missed. A drug's potential for causing drug-drug interactions is generally listed as a safety consideration; however, this case underscores the fact that such interactions can have a ripple effect throughout all the various factors we need to consider when selecting a medication: safety, tolerability efficacy, payment, and simplicity. Such interactions are frequently an important determinant of the effectiveness of the patient's entire treatment regimen rather than just the effectiveness of a single agent. Hence, they can have important implications for the quality and the cost of health care delivery. Given the varied ways that drug-drug interactions can present, practitioners should consider them in their differential diagnosis whenever a patient is on more than one medication and has a less than optimal outcome.
Another message is how physicians, by thinking about pharmacodynamics, pharmacokinetics, and biological variance (i.e., Equation 1), can more safely and effectively treat their patients whether they are using a single medication or a combination of medications. The body does not care why two or more drugs were prescribed or to what therapeutic class they belong. The body only cares whether they interact. The message here is that physicians must consider not only the drugs they have prescribed but also the other medications that the patient is taking. This issue is as important as taking patients' age and concomitant medical illnesses into account when prescribing medications for them. In essence, each medication contributes to the internal environment of the patient and may alter the patient's response to other co-prescribed medications. In this case, the patient was on antiparkinsonian medications, antidepressants, antipsychotics, and antibiotics. Despite their different therapeutic purposes, these medications interacted in a complex way to change the outcome for the patient. For this reason, one goal of rational drug development is to limit the number of sites of action a new drug affects to only those needed to treat the intended disease.14
Finally, the fact that some medications, such as fluoxetine and depot antipsychotics, take a long time to fully accumulate and clear is neither good nor bad, in and of itself. For example, depot antipsychotics were developed precisely to avoid the dangers of patients with schizophrenia, either inadvertently or intentionally, making rapid changes in their antipsychotic treatment. The longer washout period of fluoxetine probably accounts for the apparent low incidence of SRI withdrawal syndromes after its discontinuation. The clinically relevant issue is that physicians need to be aware of the time course of medications and take it into account when making treatment selections and interpreting the patient's response to treatment.
References
- Germain DM, Hughes PL, Follender AB: Potential fluoxetine-selegilene interaction. Ann Pharmacother 1992;26:1300
- Richard IH, Karlan R, Tanner C, et al, Serotonin syndrome and the combined use of deprenyl and an antidepressant in Parkinsons disease. Neurology 1997;48:1070-7
- Sternbach H, The serotonin syndrome. Am J Psychiatry. 1991;148:705-713
- Janicak PG, Davis JM, Preskorn SH, Ayd FJ Jr, Principles and Practice of Psychopharmacotherapy. 2nd ed. Baltimore, Md: Lippincott, Williams & Wilkins; 1997
- Preskorn SH, Clinical Pharmacology of Selective Serotonin Reuptake Inhibitors. Caddo, Okla: Professional Communications, Inc; 1996
- Preskorn SH, Shad MU, Alderman J, Lane R, Fluoxetine: Age and dose dependent pharmacokinetics and CYP 2C19 inhibition. Am Soc Clin Pharmacol Ther. 1998;63:166. Abstract
- Shad MU, Preskorn SH, Antidepressants. In: Levy R, Thummel KE, Trager W, Hansten PD, Eichelbaum M, eds. Metabolic Drug Interactions - Drugs as Inhibitors of Metabolic Enzymes Treatment of CNS Diseases. Philadelphia, Pa: Lippincott, Williams & Wilkins. In press
- Preskorn SH, What is the message in the alphabet soup of cytochrome P450 enzymes?. J Prac Psychiatry Behavioral Hlth. 1995;1:237-240
- Preskorn SH, I don’t see ’em. J Prac Psych Behav Hlth. 1997; 3:302-307
- Grace JM, Kinter MT, McDonald TL, Atypical metabolism of deprenyl and its enantiomer. (S)-(+)-N, alpha-dimethyl-N-propynylphenethylamine, by cytocrime P450 2D6 Chem Res Toxicol 1994;7:286-290
- Batty KT, Davis TM, Illett KF, Dusci LJ, Langton SR, The effect of ciprofloxacin on theophyline pharmacokinetics in healthy subjects. Br J Clin Pharm 1995;39(3):305-11
- Parker AC, Preston T, Heaf D, Kitteringham NR, Coonara I, Inhibition of caffeine metabolism by ciprofloxacin in children with cystic fibrosis as measured by the caffeine breath test. Br J Pharm 1994;38(6):573-6
- Preskorn SH, Harvey A, Cytochrome P450 enzymes and psychopharmacology. In: Watson S, ed. Psychopharmacology: The fourth generation of progress [CD ROM version]. Philadelphia: Raven; in press
- Preskorn SH, Reducing the risk of drug-drug interactions: A goal of rational drug development. J Clin Psychiatry 1996;57(suppl 1):3-6
-
| My columns are dedicated to my wife, Belinda, and my daughter. For this column, I owe a special thanks to Erika who convinced me to see the movie even though I thought I already knew the ending. By the way, she never told me if she wanted me to see it because it was an allegory about drug-drug interactions. |
|

