|
|
Outpatient Management of Depression
3 - How to Establish the Diagnosis in the Primary-Care Setting |
|
|
|
|
|
A challenge for the primary-care practitioner is how to
efficiently and accurately determine whether a patient is
suffering from major depression alone or in combination with
a comorbid medical illness (eg, a patient with diabetes mellitus
who is also suffering from major depression). This task is
even more challenging because there are no confirmatory or
screening laboratory tests that are sufficiently sensitive
or specific to be clinically useful. Thus, the diagnosis must
be based on clinical grounds:
- Medical history
- Physical examination
- Laboratory tests; to rule out other medical conditions
that can cause a depressive episode.
The primary presenting picture generally falls into one of
four categories:
- Mood or emotional complaints:
- Low self-esteem or feelings of inadequacy
- Anxiety
- Irritability
- Apathy
- Loss of interest
- Somatic complaints:
- Insomnia
- Fatigue
- Headache
- Weight change (loss or gain)
- "Memory" problems
- Life complaints:
- Inability to cope with marital or job stresses
- Social withdrawal or isolation
- Financial problems.
The clinician may unfortunately conclude that the depressive
symptoms are understandable results of the patient's life
situation and/or recent stressors. While that connection may
seem obvious given cultural beliefs, it is often wrong. Major
depression may be the cause of the life problems rather
than being the result of them. After all, this illness can
adversely affect work performance, motivation, and social
skills.
Having a "reason" for major depression does not
alter its course, reduce its severity and consequences, nor
change its responsiveness to treatment. Nonetheless, clinicians
may not treat major depression if they perceive that the patient
"has a reason for being depressed." However, they
would never think of not treating a myocardial infarction
or lung carcinoma because the patient has a "reason"
for having the illness, such as being overweight or being
a smoker, respectively.
Further complicating the diagnostic process is the fact
that some patients will deny the mood symptoms of clinical
depression, yet present with all the other symptoms (Figure
3.1).
What to Do After the Suspicion
of Major Depression Has Arisen
There are many possible medical causes of a depressive episode,
which need to be efficiently assessed and ruled out to arrive
at a diagnosis of major depression. The diagnostic process
can be accomplished by following these steps:
| STEP 1. |
Establish whether a depressive syndrome
is present based on eliciting the requisite signs and
symptoms (Table 1.3).
While there may be some fluctuation in the symptom severity
throughout the day or from day to day, the symptoms should
be present every day for a minimum of 2 weeks. The longer
the duration of the depressive syndrome, the less likely
it will spontaneously remit. Based on clinical trials
research, depressive episodes that have lasted for more
than 3 months are unlikely to spontaneously abate or respond
to placebo. |
| |
|
| STEP 2. |
While time is of the essence in the
primary-care setting, the confidence in the diagnosis
is higher if the patient reports the depressive syndrome
with as little prompting as possible by the clinician.
For this reason, it is preferable not to immediately go
to a litany of yes-no questions such as "have you
been having trouble falling to sleep at night?" |
The following series of hierarchically arranged questions
is recommended to establish the presence of a depressive episode:
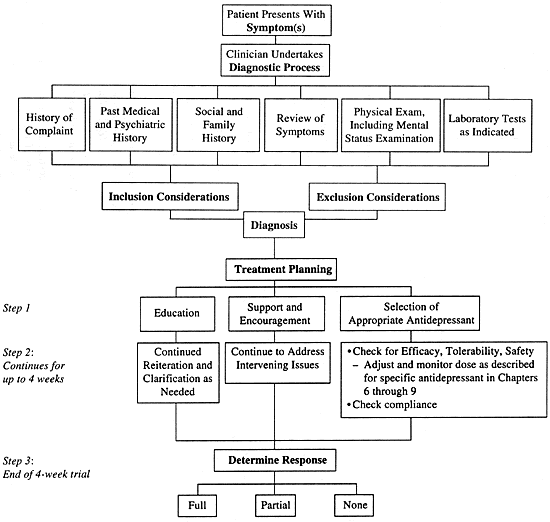
| FIGURE 3.1 Diagnostic and Treatment
Planning Process |
 |
You have been having problems with [use patient's words]
(eg, "depression," "insomnia," "stress
at work"). What else have you noticed about how you have
been feeling or acting?
This question is phrased to elicit as many
spontaneous reports of the signs and symptoms of a depressive
episode as possible. The clinician can then follow-up and
clarify the patient's answer(s) in terms of duration, clustering,
temporal stability, and severity. Frequently, a patient who
presents with mood or emotional symptoms will remain fixed
on these complaints when asked Question 1. In this case, the
clinician can move to the next more focused question.
I understand that you have been feeling [using patient's
words] (eg, "depressed," "sad," "hopeless,"
"overwhelmed"). Has this affected you physically?
This question is designed to shift the patient's mental set
to somatic signs and symptoms of major depression (ie, sleep,
appetite, energy, activity, sex drive, and concentration/attention).
The patient who has major depression will generally report
a number of these symptoms at this point. At that point, the
clinician can explore duration, clustering, temporal stability,
and severity. Based on the answers to this series of questions,
the clinician will have gathered sufficient data to have a
reasonable opinion as to whether the patient is experiencing
a depressive episode. To completely and fully assess the severity
of the syndrome, the clinician can then move to highly specific
questions, such as:
Since you have been [using patient's words] (eg, "depressed,"
"bothered by headaches"), have you also been having
problems with:
- Mood (being depressed, irritable, anxious)
- Sleep (too little or too much)
- Appetite (too little or too much)
- Energy (subjective)
- Activity (objective)
- Interest
- Motivation
- Concentration/attention
- Sex drive.
If desired, this portion can also be done by having the patient
complete a checklist or by having appropriate clinic staff
(eg, office nurse) conduct this portion of the interview.
If any answers to the questions on this list are positive
and represent new findings, further questions may be needed
to assess their duration, temporal stability, and severity,
and whether they have occurred as a cluster with any other
previously elicited depressive symptoms.
By using these three questions, the clinician can evaluate
whether the patient fulfills criteria for a depressive syndrome.
Most often, the diagnosis will be major depression. Nonetheless,
a depressive syndrome can be due to several other causes.
Hence, the clinician needs to rule out other possibilities.
Work-Up for Other Causes of a Depressive
Syndrome
(Table 3.1)
- Medical history and physical examination-the clinician
can assess for a variety of other medical causes of major
depression
- History of present illness-be alert for any signs of symptoms
that are not typically associated with major depression
(eg, productive cough)
- Past medical history-are there any past illnesses that
could be recurrent and cause a depressive syndrome?
- Medications-is the patient taking any medications (eg,
antihypertensives, steroids) which could cause a depressive
syndrome?
- Social history-is the patient drinking alcohol or abusing
illicit drugs?
- Family history-are there other family
members with major depression or other psychiatric disorders
that could be presenting as a
depressive syndrome? Remember most psychiatric illnesses
run in families. The family history therefore can help elucidate
and support the diagnosis. Conditions such as somatization
disorder (eg, Briquet's syndrome) can present with waxing
and waning complaints of dysphoria and anxiety and lead
to a false-positive diagnosis of major depression. Somatization
disorders tend to run in families, so check whether other
relatives (particularly females) have complicated medical
histories. A family history of bipolar disorder increases
the likelihood that the patient will eventually have a manic
episode, and treatment with a mood stabilizer (eg, lithium)
might be warranted, either alone or in combination with
an antidepressant (Chapter 11).
- Physical observation-the patient with major depression
typically will have the following findings (Figure
3.1 and Table 3.2):
- Diminished eye contact
- Sad, apathetic, or emotionally blunted expression
- Stooped posture
- Decreased rate and rhythm of speech
- Increased latency of response.
Less often, patients will show:
- Irritability
- Psychomotor restlessness (eg, drumming fingers, biting
nails). The efficient clinician can assess the mental status
while obtaining the history and will also be comparing the
patient's subjective statements about the severity of the
patient's condition with observations of behavior during
the interview.
- Laboratory tests-the standard laboratory
work-up is to evaluate other possible medical causes. These
tests include:
- Complete blood cell count
- Liver, renal, and thyroid function tests
- Urinalysis
- Serology for infectious diseases (if the history warrants).
Other laboratory tests would be more patient specific, such
as an electrocardiogram, depending on the age of the patient,
or brain imaging if a neurological condition needs to be
assessed.
| TABLE
3.1 Typical Behavior During Office Visit |
| Behavior |
Depressed
Patient |
Not Depressed
Patient |
| Affect |
- Sad/anxious affect
- Sad/anxious expressions
- Stooped, sagging posture
- Frequent negative statements
|
- Predominantly positive affect
- Full range of affective expressions
- Facial animation
- Frequent positive and affect-laden expressions
|
| Rate of behavior
|
- Decreased rate of behavior
- Speaks less often
- Speaks with less intensity
- Looks at others less
- Less spontaneous
|
- Sustained, spontaneous, and appropriate goal-directed
behavior
|
| Responsiveness |
- Responses slow and halting
- Frequent nonacknowledgment
- Sadness and withdrawal in response to
anger or irritation in others
- Critical of others
|
- Normal rate and rhythm of response
- Responses affectively appropriate
|
| Tolerance |
- Frequently irritable/hostile, especially
in intimate relationships
- Low stress tolerance
- Irritability increases as stress increases
|
|
| Adaptation to stressful
situations (eg, work, home) |
- Uses strategies requiring least cognitive
effort
- Forced obedience
- Withdrawal in face of resistance
- Benign neglect
|
- Able to negotiate solutions
- Attentive to behavior and contingent responses
- Able to foster sustained positive interactions
|
|
| |
|
| TABLE 3.2
Varied Terms Used for Depressed Mood |
| Depressed Person May Report
Being: |
Others May
Describe the Depressed Person as Being: |
| Down |
Gloomy |
| Sad |
Pessimistic |
| Unhappy |
Cynical |
| Discouraged |
Grim |
| Empty |
Negative |
| Miserable |
Moody |
| Beaten |
Serious |
| Defeated |
Stern |
| Hopeless |
Severe |
| Helpless |
Oppressive |
|
For the primary-care clinician who has
treated the patient for some time, the above history may either
already be known or can be quickly elicited. If that is not
the case, then the clinician or a staff member can obtain
that information at either the initial or a follow-up visit.
That decision should be based on the clinician's assessment
of how likely it is that this information would substantially
alert his/her opinion and course of treatment.
Note: The above has focused on differential diagnosis
and thus has discussed major depression and other medical
conditions from an "either/or" perspective. In fact,
clinical depression is frequently comorbid with a variety
of other medical illnesses (eg, cancer, diabetes, coronary
artery disease). In such instances, both conditions need to
be treated for optimal outcome. Otherwise, untreated clinical
depression can seriously compromise the ability to effectively
treat the whole patient. This fact also means the clinician
needs to be mindful of the potential for interactions between
the various medications the patient will be taking. This issue
and its relevance to antidepressant drug selection is discussed
in greater detail in Chapters 6
and 10.
To Treat or Not to Treat Now?
If the severity of the syndrome is mild and/or not convincingly
present, the clinician may decide to defer initiating antidepressant
pharmacotherapy and schedule the patient for a follow-up within
1 week. This approach permits an assessment of the temporal
stability of the patient's complaints. That is particularly
true if somatization disorder is suspected because depressive
and anxiety complaints in such patients may be prominent one
week and gone the next.
Conversely, if the illness is sufficiently severe to be
causing distress and/or dysfunction, the prescriber may elect
to start a trial of medication, and schedule a follow-up visit
in 1 week. Chapters 6 through 9
provide a way of evaluating which antidepressant is likely
to be the best option for a specific patient.
|

